5 New Non-Drug Treatments to Watch
As more resources are devoted to creating remedies for the opioid epidemic, healthcare technology manufacturers are looking to create and improve non-pharmacologic solution for pain management and treatment. Whether they’re just now coming into the mainstream or recently developed, here are five treatments that are seeking to curb the overuse of opioid painkillers.
1. Spinal Cord Stimulation
Effective for: Chronic back, leg, and arm pain
Other potential applications: FBSS, neuropathy
How it works: Spinal cord stimulation is a treatment for relief of chronic pain that delivers a low-voltage electrical current to the spine to block the sensation of pain. Delivered via an implanted device, this electrical current prevents signals that would trigger a pain response from reaching the brain. This can result in pain reduction from 50-75%, which can mean the difference between ability and disability in a patient with chronic back pain.
In the past, spinal cord stimulation has been considered a last-resort treatment for chronic back pain, to be recommended only after other treatments, including surgical correction, have failed. However, with increased pressure from government bodies and healthcare professionals alike to prioritize non-drug treatments for pain over opioid drugs, spinal cord stimulation has begun to emerge as a recommendation for managing chronic pain earlier in the treatment process. It may not be effective in every case, however, due to the inherent risks.
Risks or drawbacks:
- Efficacy: Spinal cord stimulation is determined successful if it reduces 50% of the patient’s pain, and in some cases, may have less effect, or none at all.
- Overstimulation: For some patients, the electrical current creates an unpleasant buzzing sensation in the spine.
- Malfunction: Impacts can dislodge the lead from the device, which requires surgery to reattach.
- Risks associated with surgery: Spinal cord stimulation devices require several surgeries for testing, implementation, and maintenance, increasing any possible risk of surgery, such as infection and blood clots.
- Risks associated with electroanalgesia: Spinal cord stimulation is dangerous for patients who need other electrical equipment in their bodies, such as pacemakers and hearing aids. The electrical signals from different devices may interfere with one another and fail.
2. Vagus Nerve Stimulation
Effective for: Epilepsy, depression
Other potential applications: Headaches, multiple sclerosis, pain, Alzheimer’s Disease
How it works: Vagus nerve stimulation, like spinal cord stimulation, delivers a low-voltage electrical current to an area of the nervous system—in this case, the vagus nerve. Implanted vagus nerve stimulation devices have been used to treat epilepsy that does not respond to other treatments, reducing the number of seizures that a patient experiences by 20-50%. It is also used, more controversially, for patients with hard-to-treat depression, for whom results are mixed.
More recently, non-invasive vagus nerve stimulation devices, such as gammaCORE, have been developed and studied for treatment of migraines, cluster headaches, chronic pain, and Alzheimer’s Disease.
Risks or drawbacks:
- Side effects: A few health problems and side effects associated with vagus nerve stimulation are voice changes, cough, tingling, chest pain, difficulty swallowing, and bradycardia (slowed heart rate).
- Risks associated with surgery: Only implanted vagus nerve stimulation devices are currently approved for use in the United States, though non-invasive devices are approved for use in Europe. Therefore, any possible risk of surgery, such as infection and blood clots, are possible when implanting the device.
- Risks associated with electroanalgesia: Vagus nerve stimulation is dangerous for patients who need other electrical equipment in their bodies, such as pacemakers and hearing aids. The electrical signals from different devices may interfere with one another and fail.
3. Transcutaneous Electrical Neural Stimulation (TENS)
Effective for: Chronic musculoskeletal pain, post-operative pain
Other potential applications: Labor pain, migraines
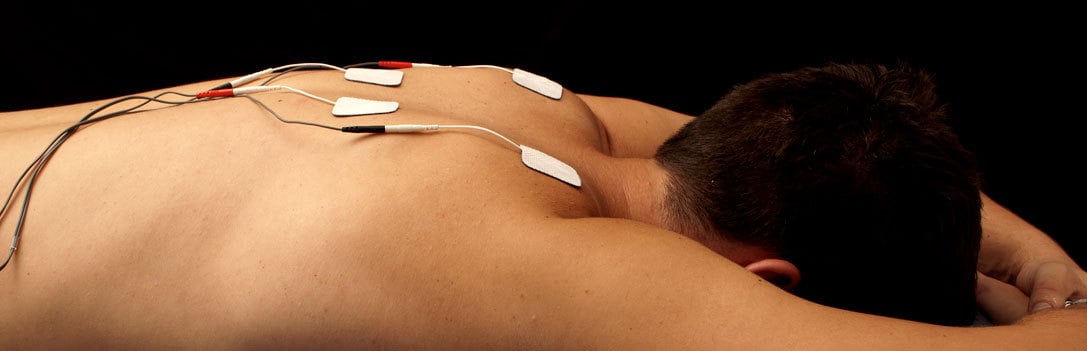
How it works: The third form of electroanalgesia differs from both spinal cord stimulation and vagus nerve stimulation in that TENS is, by definition, non-invasive. Typically, a small TENS unit is connected to the skin using two or more electrodes, through which pulsed electric currents are delivered directly to the area from which a patient’s pain originates.
TENS benefits from having few—if any—risks for qualified patients. However, it is more suitable for the relief of light to moderate pain, and may not have the desired effect for sufferers of debilitating chronic pain. Regardless, it is a treatment that has been receiving more attention as a front-line option for pain management, and further research and improvements could prove critical in the response to the opioid epidemic.
Risks or drawbacks:
- Tolerance: TENS treatments lasting more than a few minutes will decline in efficacy as the patient becomes accustomed to the pulses. It is easy, therefore, to “max out” the intensity of a unit and limit the pain relief the patient experiences.
- Risks associated with electroanalgesia: Cases in which a patient with a cardiac pacemaker has been treated with TENS around the area where the device is implanted have resulted in device failure. Therefore, TENS is not recommended for patients with existing implanted devices.
4. H-Wave Electrotherapy
Effective for: Chronic pain, muscle spasms, post-operative pain
Other potential applications: Anesthesia
How it works: H-wave electrotherapy is often compared with TENS, due to similarities between the devices in both looks and usage. However, H-wave electrotherapy is distinct in its ability to treat pain, not simply block or manage it. It induces non-fatiguing contractions on the site where electrodes are placed, increasing circulation for natural healing and rehabilitation.
Because H-wave electrotherapy is synonymous with the H-Wave Device, developed by Electronic Waveform Lab, Inc., all research and results are based on the same device, which has only two settings. Despite, or perhaps because of, its simplicity, practitioners and patients alike who are interested in electroanalgesia have praised the H-Wave’s efficacy.
Risks or drawbacks:
- Price: While the price for clinical units is comparable to other electroanalgesia technology, the unit sold for home use is only slightly cheaper. Combined with the fact that it is not covered by all insurance carriers, patients wishing to manage chronic pain at home face a steep cost.
- Risks associated with electroanalgesia: Like with TENS, H-wave electrotherapy is best avoided for patients with existing implanted devices.
5. Virtual Reality
Effective for: Acute pain (especially during medical procedures such as wound care, chemotherapy, and dental procedures)
Other potential applications: Chronic pain management
How it works: Unlike the other treatments on this list, the pain relief provided by virtual reality (VR) treatments is purely psychological. While psychological methods for treating pain, such as keeping patients informed about their conditions and treatments and cognitive behavioral therapy, are used regularly today, VR technology allows medical professionals to further explore the ways that humans experience pain.
Since 1996, VR has been used to manage acute pain during medical procedures. Recently, however, medical professionals have been exploring the possibility of VR as a treatment for chronic pain. It currently works primarily as distraction, so the brain focuses less on pain and more on the immersive environment. However, VR neurotherapy is a growing technology that teaches patients’ brains to relearn how to react to pain signals, thereby reducing overall pain.
Risks or drawbacks:
- Price: VR hardware that is intended for mass consumption, such as gaming consoles and education platforms, may not inspire patient confidence in the treatment, and sophisticated systems may be cost prohibitive to wide scale research and use in medical settings.
- Lack of evidence: Though the use of VR for management of acute pain, especially during medical procedures, is well researched and effective, applications for the management of chronic pain are still being investigated.
As healthcare professionals and patients demand more non-drug pain management options, healthcare technology developers are searching for new and improved ways to meet the need. With a diverse array of treatments for different conditions, an industry that considers pain medication only as a last resort is on the horizon—and the change couldn’t come sooner.